Cessation Techniques
To Help Someone Quit Chewing Tobacco
Cessation techniques
2. Quitting “Cold turkey”- People can and do quit chewing on their own. The health professional can be very helpful by encouraging quitting and giving support whenever possible. Chewers who have not been chewing very long are often successful with this method.
3. Chewing an alternative- Oral gratification “missing having something in my mouth”, behavioral rituals and peer pressure are powerful influences to keep a person using smokeless tobacco. Here is where using healthy alternatives like Mint Snuff All Mint Chew or Pouches becomes so valuable. They allow the patient to continue the behavior and yield to whatever pressures keep them chewing but without the danger of tobacco. Some people can quit the behavior altogether after a few weeks, others take longer. If they quit and then feel the need to relapse, they can once again use Mint Snuff until the urge passes.
4. Titration- Some chewers who have strong nicotine withdrawal find it helpful to mix Mint Snuff with their tobacco. Some mix it with tobacco in a ratio of 1:4 one week, 1:3 the following week, 1:2 the next, 1:1 afterwards and finally to straight Mint Snuff. Click here to see Dr. Dan Laizure’s method.
5. Alternating dips- Use tobacco and Mint Snuff alternately starting every other dip then gradually using Mint Snuff more and more until they don’t use tobacco anymore.
6. Use of nicotine patches- For those chewers who display definite signs of nicotine withdrawal, doctors may consider the use of nicotine patches. Please check the latest information on suggested levels and age criteria for the use of patches with smokeless tobacco users.
7. Nicotine gum (Nicorette)- Studies have suggested that nicotine gum has not been very helpful in the cessation efforts. However, it is always worth a try if the patient wants to try it.
8. A prescription of wellbutrin (also called Zyban, a prescription anti-depressant pill) and the use of Mint Snuff Chew or Mint Snuff Pouches. A few un-named professional baseball players quit using this method.

Intervention techniques
One of the most difficult things to deal with when intervening with a patient about tobacco use is how and when to do it. Until now, just telling a patient that they should quit chewing and not offering any assistance or alternatives created some stress for the patient. By offering an alternative, you can now establish a good relationship and give the patient something to use in their own quitting process. When combined into a comprehensive intervention plan, the overall effect towards ultimate cessation can be quite effective. Here are some other suggestions of how to deal with different patient ages:
- Be consistent- Ask every patient (especially adolescents) on each visit if they use tobacco. If they don’t, praise them for non-use and urge them to continue avoiding tobacco. If they do chew, briefly inform them of the dangers of tobacco, provide them literature and ask them if they want to quit. Consistently asking someone about their tobacco use, especially young adults, offers many opportunities for intervention.
- Kids from about 8yrs to 14yrs- These kids can be some of our best ambassadors of health! You may want to ask them if they use tobacco in either a direct or offhand manner: “I assume you are still not using tobacco, right?” or “How do you feel about kids who are using chewing tobacco?” Ask their opinion about tobacco use and if they know others who chew tobacco. Whatever answer they give you can lead to an intervention opportunity:
- “No, I don’t use tobacco”- Your response- “Wonderful, and I don’t ever want you to begin..” Some have expanded this opportunity to ask if they know about the dangers of chewing tobacco so they might be able to tell one of their friends that does use tobacco. Ask if they would like to take some brochures on tobacco cessation to a friend. By intervening now, and letting them know how you feel about tobacco use, they can begin creating an anti-tobacco attitude before they are offered tobacco from a peer or another adult!
- “Yes, I have (or do) use chewing tobacco” – It can happen! The best you can do now is to find out how much they are using, why and then tell them briefly about the dangers of tobacco and that they should think about making their own decision to quit. There are no good reasons for them to be chewing tobacco. Offer them information about the dangers of tobacco and try to find out why they chew.
- Kids from about 14yrs to 21 yrs- Sometimes this is the toughest group to get to but represent the majority of new users. Asking if they would like to quit and then giving them information about the dangers of tobacco use are a great way to begin. If it is obvious that they are probably going to continue “dipping” anyway, you might want to suggest they do so with a healthy and harmless product like Mint Snuff and offer them a sample can.
- People 21 yrs and older- Many of the chewers in this age group have been chewing for many years. However, they may have also read about the dangers of chewing and/or have had their girlfriends or wives urge them to quit. For whatever reason, the health professional can again ascertain their desire to quit and offer an alternative if they need one. These people may need extra help with nicotine withdrawal.
- Kids from about 8yrs to 14yrs- These kids can be some of our best ambassadors of health! You may want to ask them if they use tobacco in either a direct or offhand manner: “I assume you are still not using tobacco, right?” or “How do you feel about kids who are using chewing tobacco?” Ask their opinion about tobacco use and if they know others who chew tobacco. Whatever answer they give you can lead to an intervention opportunity:
- Find out if the patient is ready to quit- If the patient uses tobacco, tell them of your concern that they quit and ask them, “Do you want to quit?” If the answer is YES, continue with the cessation program. If their answer is NO, state “When you want to quit, let me know and we can help,” then go on with your normal procedures. Don’t badger, just let them know that you care and you can help. Cessation experts report that unless a person is ready to quit, your chances of helping them is very low.
- Offer help- If your patient uses smokeless tobacco, ask them why they chew, and if they would be able to quit “cold turkey.” Ascertain whether or not they chew for social and/or behavioral reasons (i.e. “other guys do it…,” “only during baseball..,” “I need something in my mouth..,” etc.) If they feel like they want to continue chewing but need help with their behavior by using an alternative, offer Mint Snuff™ All Mint Chew™ or All Mint Pouches™.
Where Can You Send Patients to Buy Mint Snuff?
Mint Snuff Chew™ and Mint Pouches™ are usually found in the tobacco section at grocery and convenience stores. Many Krogers and Kmarts now carry Mint Snuff Chew and Mint Snuff Pouches. Please ask your favorite store to carry it for you or your patients. For a store near you click here or call 1.800.EAT.MINT * 1.800.328.6468 8:30a-5:30p Pacific Time Mon.-Fri.

$1 Mint Snuff Pouches Samples Available
Consumers may order samples of Mint Pouches for $1.
If you are going to have a special promotion such as a health fair or other tobacco-related event, please call the Oregon Mint Snuff Company at 1.800.EAT.MINT * 1.800.328.6468 with your ideas. Practice SAFE SNUFF with Mint Snuff.
Prevention Is The Best Medicine
Prevention is the best medicine!
It is easier to try to prevent a person from ever using tobacco than trying to get them to quit once they have begun.
However, some tobacco chewers, especially children and adolescents, don’t comprehend tobacco dangers until they are into their late teens if at all and by that time might have been chewing for five or ten years.
Research suggests the success rate for tobacco cessation in a health practitioner’s office is somewhere around five percent. But that does not mean that there is a ninety-five percent failure rate!
The person who receives the quit message may not, and probably won’t, quit immediately, but, he may get the same message from others like a nurse, his wife, a friend or others and later reflect about what was told to them.
Eventually, after many intervention episodes, the patient may make his own decision to quit and often comes back to the dentist or hygienist for help in doing so.
Health professionals shouldn’t grade themselves on how many people they can “get” to quit, but rather how many times they give the message when the opportunity arises.
Under these criteria, there is no reason not to have an intervention success approaching 100%. Once the patient has made the decision to quit, then the professional should be ready with suggestions.
Smokeless Tobacco Intervention and the Health Professional
While about 75% of health providers think it is a good idea to tell patients about tobacco dangers, only about ten percent routinely do so. Research shows that the reasons they don’t get involved are a combination of not feeling confident about the subject, questionable goals of doing so, afraid of a negative reaction from the patient, feel that the patient would be offended, there is not enough reimbursement to get into cessation or they just don’t have enough time.
Kids hear about chewing tobacco at an early age due to tobacco advertising, store displays, friends and even unknowing parents introduce smokeless tobacco to some kids as young as 3 to 9 years.
By the time a child is ten, they may know what smokeless tobacco is but they may not understand what the dangers are.
When a health professional asks a child if they know about, or even use smokeless tobacco, a golden intervention opportunity exists.
When a health professional identifies that a patient is using tobacco, there are many intervention opportunities available.
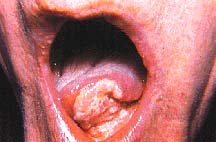
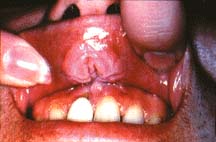
The obvious one is to show them how evident it is that they chew tobacco by pointing out gum recession, tooth decay, leukoplakia or other histological effects caused by tobacco use and offering a brief message that they should quit.
Graphic pictures, brochures, videos or other information could be provided, depending on the time available and receptiveness of the patient.
Asking whether or not they know how dangerous spit tobacco is, often brings the surprise reaction that they don’t know that smokeless is a health risk.
If the patient doesn’t use tobacco, a professional can take a moment to congratulate them for non-use, tell them their own position on the use of tobacco, and solicit a promise from them that they will never use tobacco. If we can keep a child away from tobacco until they are about eighteen, there is a very good chance that they will never use tobacco.
Research shows that one of the main reasons young people start using tobacco is social pressures or imagery.
Kids usually get their first “dip” from a friend or family member. Shockingly, some kids have admitted they are willing to risk their health in order to have the circle on their back pocket or to just “fit in” with other young chewers. Trying to compete against this peer pressure or social imagery can be perplexing for health advisors.
The Role of an Alternative
Dealing with the social and behavioral aspects can be tough. For kids who chew for social or image reasons, a professional can either try to convince them to quit “cold turkey” or offer an alternative that provides them the same social imagery and behavior but is harmless.
Some of these alternatives are sunflower seeds, bubble gum and sugarless candy which, although somewhat acceptable, don’t offer the same perceived benefits as their chew.
Two alternatives which are safe, food grade products are Mint Snuff All Mint Chew and Mint Snuff Pouches produced by the Oregon Mint Snuff Company (1-800-EAT-MINT; www.mintsnuff.com ). These products are made from mint, not tobacco and offer the same look, feel and behavior as tobacco.
By giving a chewer Mint Snuff, a professional is meeting the user “half-way” and providing a positive experience during the intervention phase. Naturally, it’s better if the chewer didn’t do the behavior at all, but if they are going to chew anyway, it’s better they used mint instead of tobacco.
The availability of an alternative greatly increases the health professional’s chances of helping their patients quit tobacco. Rather than hand-wringing and chanting “you should quit” they can say: “try this!”
From November 1990 through December 1998, the Oregon Mint Snuff Company has given over 1 million free cans of non-tobacco chew as well as thousands of educational posters and brochures to dentists, hygienists, county health departments, and other health professionals. Over 10,000 dentists, hygienists, and other health professionals have received samples and recommend Mint Snuff to their patients.
Cessation Methods
Why do people chew tobacco? There is no one way to help people quit chewing tobacco just as there is no one reason they chew. Like cigarettes, there seems to be the same three main reasons for chewing: social/psychological, behavioral and physical (nicotine addiction).
Different social, cultural and behavioral influences have raised new challenges for intervention and cessation techniques. A cessation method that works in one state or community may not work in another. For instance, a young chewer in North Carolina might, sociologically, have radically different needs than a chewer in Arizona because tobacco is part of the economic base of the community. “Uncle Joe grows tobacco…it can’t be bad!”
Another interesting example is Alaskan Indians, who would use Mint Snuff instead of tobacco as long as it was provided free – but when they had to pay any amount of money for it, would chew tobacco instead.
In order to address all three aspects of the chewing behavior (physical, psychological and social) while at the same time being sensitive to different cultural demands of various societies, we have listed a compilation of ideas we’ve collected here: Developing a Cessation Program For Your Clinic and Personal use
Turning Smokeless Tobacco Intervention into a Practice Builder
Smokeless tobacco intervention can be a good practice builder. Health practitioners offer help to people for a problem that is widespread and lacks conventional assistance. Quite often the person asking for help is not the chewer, but rather a parent or friend who wants to help someone they know quit tobacco.
Dental practices that let their community know that they are concerned and have possible solutions to this problem are doing great public relations and a great public service.

